Resident Author: Jennifer Rabjohns
Faculty Mentor: Massoud Kazzi
Date of Presentation: 12/27/2018
Introduction:
70yoM p/w exertional fatigue, altered mental status, and BP 80s/50s. Hx significant for head and neck cancer complicated by recent CSF leak.
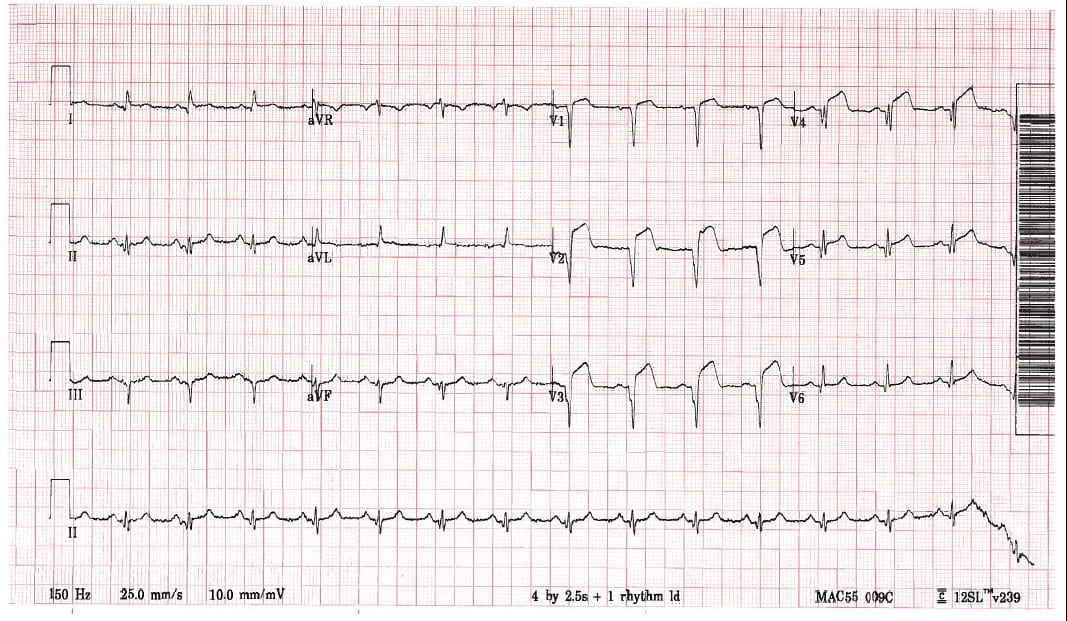
EKG is below:
How would you describe this EKG?
Inferolateral ST segment elevations with aVR depression.
What is the differential diagnosis?
When seeing AMS and hypotension, remember your causes of shock: hypovolemic, distributive (sepsis, anaphylaxis), obstructive, neurogenic, and cardiogenic. The recent CSF leak with concern for sepsis was a red herring! EKG showed STEMI.
Background on Ischemic EKG Changes:
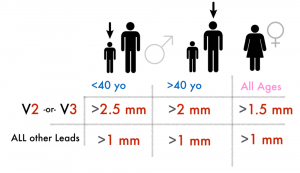
In August of 2018, the Fourth Universal Definition of Myocardial Infarction was published, which included EKG changes suggestive of ischemia ():
We'll talk about ST elevation here.
A review: The J-point is the start of the ST segment. Compare it to the T-P segment (ST Morphology).
Some sources (including the above) recommend comparing the J-point to the P-R segment, but pericarditis (PR depression) can make things confusing, and T-P is generally isoelectric.
Now, ST elevation suggestive of ischemia is defined as 1 of 2 things:
1.) 1mm in 2 contiguous leads except for V2 and V3. Remember our example from this case:

2.) Specific ST elevations in V2 or V3
(STEMI and STEMI Equivalents 2015).
In the next example, the STE actually extends beyond V2 and V3.
However, STEMI's only account for 25% to 40% of presentations of MI (Tamis-Holland 2014). This is consistent with the table above, which mentions ST depression and TW inversion as possible evidence of ischemia. But from the 2017 European Society of Cardiology Guidelines for the Management of STEMI, patients may have coronary artery occlusion or global ischemia without ST-elevation if there is:
- bundle branch block
- ventricular pacing
- hyperacute T waves
- isolated ST-depression in anterior leads, and/or
- universal ST-depression with ST-elevation in aVR.
Those ESC guidelines state that in patients without ST elevation, but who have "the [above] mentioned electrocardiographic (ECG) changes and clinical presentation compatible with ongoing myocardial ischemia, a primary percutaneous coronary intervention (PCI) strategy (i.e., urgent angiography and PCI if indicated) should be followed" (Kala 2017).
Take-home points:
- Look for the ST elevation criteria if you have suspicion.
- Keep an eye out for MI without ST elevations and consult cardiology as needed.
Case Resolution:
Cath attack was called. Cath showed 3-vessel disease: 100% occlusion in LAD, 99% in circumflex (received BMS), 99% in RCA (received BMS). Pt transiently had IABP, RV Impella, and was on multiple pressors; he was successfully weaned off of these and discharged home.
References:
- Kala, P., Mates, M., Zelizko, M., Rokyta, R., & Ostadal, P. (2017). 2017 ESC Guidelines for the management of acute myocardial infarction in patients presenting with ST-segment elevation. Summary of the document prepared by the Czech Society of Cardiology. Cor Et Vasa, 59(6). doi:10.1016/j.crvasa.2017.10.008
- ST Morphology. (n.d.). Retrieved December 27, 2018, from https://en.ecgpedia.org/wiki/ST_Morphology
- STEMI and STEMI Equivalents, i.e. Who Needs the Cath Lab Now! (2015, August 31). Retrieved December 27, 2018, from http://www.tamingthesru.com/blog/grand-rounds/stemi
- Tamis-Holland, J. E., & Ogara, P. (2014). Highlights From the 2013 ACCF/AHA Guidelines for the Management of ST-Elevation Myocardial Infarction and Beyond. Clinical Cardiology,37(4), 252-259. doi:10.1002/clc.22258
- Thygesen, K., Alpert, J. S., Jaffe, A. S., Chaitman, B. R., Bax, J. J., Morrow, D. A., & White, H. D. (2018). Fourth Universal Definition of Myocardial Infarction (2018). Journal of the American College of Cardiology, 72(18), 2231-2264. doi:10.1016/j.jacc.2018.08.1038